|
However, it remains elusive if the elevated NSE levels in the patient's serum belong to the adenocarcinomas, the DIPNECH lesions or a combination of both. Interestingly, besides typical carcinoid markers such as CD56, synaptophysin, and chromogranin A, the DIPNECH lesions were also positive for NSE. The adenocarcinoma was positive for typical markers such as CK7, CK18, TTF1, and SPA and additionally, it was positive for NSE and CEA, which were also measured to be elevated in the patient's serum. The current report represents the first case of a patient with DIPNECH accompanied by a pulmonary adenocarcinoma of mixed subtype with partial neuroendocrine differentiation. We have recently reported a similar case in which DIPNECH was associated with a carcinoid. Only 3 of these 1090 cases were associated with DIPNECH and the primary tumors were carcinoids in all of these cases. In a recent study including 1090 patients, who received resections for primary lung tumors, Ruffini and colleagues found that the overall prevalence of pre-invasive lesions for lung carcinomas was 6.7%. However, it has become generally accepted that DIPNECH is a precursor to pulmonary carcinoid tumors. Only 40 cases of DIPNECH have been reported in the literature to date and there are no predictive histological or genetic data available so far. Due to its neuroendocrine origin, its similar morphology to pulmonary carcinoids and particularly due to its association with pulmonary carcinoids, the disease is considered to be a precursor lesion for theses entities. Six months after the operation the patient is still alive and no tumor recurrence has been detected so far.ĭIPNECH is an exceedingly rare disease involving generalized proliferation of pulmonary neuroendocrine cells, which leads to an occlusion of the bronchial lumina and consequent clinical symptoms such as shortness of breath. The postoperative course of the patient was uneventful. There were no clinical symptoms suggestive of any proteins and/or hormones released, but interestingly, NSE (20 ng/ml) and CEA (33 ng/ml) were slightly elevated, whereas Cyfra was within the normal range (1.4 ng/ml). Due to the multicentricity of the lesions and a size of 5 mm are classified as carcinoids according to the current WHO classification. 
Therefore, the diagnosis of multiple tumorlets (microcarcinoids) was made. In these lesions, the cells were strongly positive for CD56, synaptophysin, NSE and chromogranin A and focally positive for CK7, CK18, TTF1 with a proliferation rate (Ki67) of 1–2%. However, further processing of the multiple small lesions in the upper and middle lobe revealed five foci less than 5 mm in diameter with a different trabecular and nest-like morphology (Fig. Therefore, the TNM classification for the pulmonary adenocarcinoma was pT4, pN2 (16/27), pM1, G3. Tumor infiltration of intrapulmonary and mediastinal lymph nodes was also present. Besides this main tumor there were multiple small metastases with a similar degree of differentiation in the upper right lobe as well as in segment 4 of the middle right lobe. The proliferation rate (Ki67) was 20–30%. The tumor was strongly positive for CK7, CK18, TTF1 and SPA and focally positive for CEA, NSE and chromogranin A. 
Pathological processing of the specimens revealed a 3.5 × 3 × 2.8 cm adenocarcinoma of a mixed subtype with partial neuroendocrine differentiation (Fig. Since the CT findings raised the suspicion of a malignancy, a diagnostic thoracotomy with a concurrent sleeve lobectomy of the right upper lobe was performed in combination with a systematic lymphadenectomy. Pre-operative diagnostics revealed arterial hypertension and moderate left ventricular hypertrophy and pulmonary function tests were unsuspicious (VC 143%, FEV1 128%). 
The patient had a 10 pack-year smoking history and complained of shortness of breath upon admission the remaining review of symptoms was negative. 1) was indicated following detection of a pulmonary nodule in the right upper field on routine chest -x-ray. These lesions were suggested to represent metastases of the lesion in segment 2. Additionally, several lesions as large as 0.6 cm were evident in segments 4 (right middle lobe, lateral segment) and 6 (right lower lobe, superior segment) of the right lung. The 60-year-old female patient was initially referred to our hospital because computed tomography scans revealed a tumor-like lesion measuring 2.9 cm in its widest diameter in segment 2 (right upper lobe, posterior segment) of the right lung. 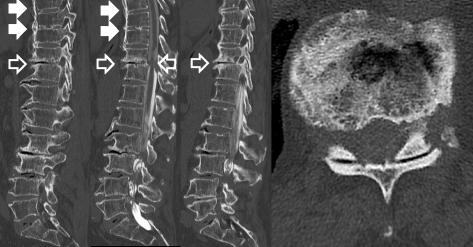
Here we report on a patient with DIPNECH who coincidently developed a pulmonary adenocarcinoma.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
